Cardiac Rhythms
Part 1
- EKG Rhythms are often named according to the source of the electrical activity in the heart or the structure where the problem is occurring.
- Pacemaker Rhythms are aptly named due to the locus of stimulation coming from an artificial impulse generator called a pacemaker.
- The most common pacemakers may deliver an electrical impulse to the right atrium, right ventricle or both.
- Artificial pacemakers are often implanted as a result of either a failure of the higher (faster) pacemakers within the heart or an irregular rhythm resulting in decreased cardiac output.
- Remember, the fastest electricity in the heart (regardless of location or source) will dictate the heart rate.
Part 2
- Each EKG rhythm strip in this category will share unique a morphologic feature which separate them from all other rhythms.
- Pacemaker rhythms are identified by the presence of a conspicuous vertical mark known as a “spike”.
- If the spike precedes the P wave, it is referred to as an Atrial Pacemaker rhythm.
- If the spike precedes the ventricular depolarization, it is referred to as a Ventricular Pacemaker rhythm.
- If there is a spike prior to the P wave and the ventricular depolarization, it is referred to as an AV (atrioventricular sequential) Pacemaker rhythm.
-
Note: QRS complexes in Ventricular and Atrioventricular
Pacemaker rhythms will have a wide, bizarre appearance (just like
ventricular rhythms) and typically measure 0.12 seconds or greater.
- After learning the unique features just described, it is simply a matter of recalling the unique feature and associating it with the corresponding waveform.
Part 3
- During implantation, pacemakers are programmed by the physician to provide electrical impulses at a specific strength of impulse (enough to cause depolarization) and with a certain rate to maintain cardiac output within a specific normal range.
- Many pacemakers also are programmed to “sense” the inherent electrical activity occurring within the heart, so the device only turns on when needed and does not compete with the patients own natural electrical activity.
- Sensing capability is an important safety feature in pacemakers to ensure the electrical impulse provided by the pacemaker does not inadvertently occur during the vulnerable period of repolarization (relative refractory period).
Part 4
-
Unfortunately not all pacemakers work the way they should.
According to Pub Med, an article titled “Complications related to permanent pacemaker therapy” (http://www.ncbi.nlm.nih.gov/pubmed/10353129): In a group of patients studied at Kuopio University Hospital, inadequate capture or sensing was observed in 7.4% of the patients.
- A variety of problems can occur when is comes to pacemakers. The wire may not embed in the endocardium or pull out post-procedure, the device may oversense or undersense or fail to capture.
|
|
Introduction
Part 1
- Basic principles of rhythm analysis require an understanding of speed and voltage (amplitude).
- Standard recording speed is 25 mm/sec.
- It is important to remember this unit of measure because it lends consistency to measurement when analyzing interval, complex and segment durations.
Part 2
- If the print speed is increased or decreased, it will not only affect the distance of one cardiac complex to the next, it will affect the measurement duration of critical aspects of the cardiac complex.
- Paper speed is often marked on the tracing. It is important to check this setting prior to printing and analyzing any tracing.
Part 3
- Voltage is represented vertically in the cardiac tracing.
- Standard calibration or gain is set at 10 mm/mV. It is important to remember this unit of measure because it lends consistency to measurement when analyzing the height and depth of cardiac waves.
- If the gain is increased (20 mm/mV) or decreased (5 mm/mV), it will affect the size of the waves in a cardiac complex. This can be a useful feature when a patient’s cardiac tracing is either too small to analyze effectively or so large that the waveforms are overlapping or tracing off of the paper.
Part 4
- It is important to be aware of the settings on the equipment you are working with daily.
-
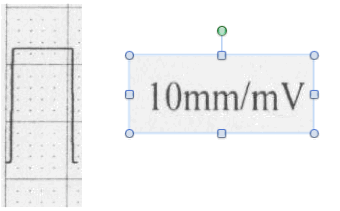
Many times a calibration pulse is seen at the beginning, end or both on a cardiac tracing (it looks like a rectangle about 5 mm wide and 10 mm tall in “standard calibration”). Some units will simply print 10 mm/mV on the bottom or top of the tracing, some machines will do both. Make sure you are familiar with your equipment.
 |
|
Graph Paper
Time 1
- The value of time and voltage just discussed is very important to understand, but it must be combined with an understanding of the grid or graph paper the tracing is printing upon that you are analyzing.
- The grid is broken down in small boxes (1 X 1 millimeter) and heavier darkened lined boxes.
- There are five small boxes going from left to right and bottom to top of each large box (5 X 5 mm).
Time 2
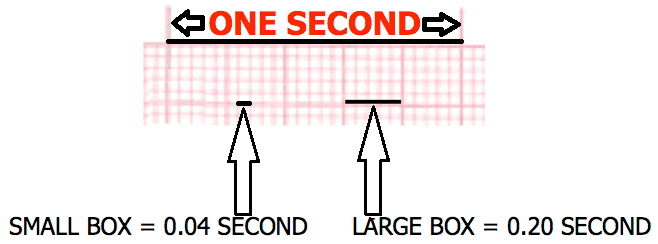
- Each small box has a time value of 0.04 second.
- If there are five small boxes going across each large box, then the value of time for each large box equals 0.20 second
- (5 small boxes X 0.04 second = 0.20 second)
- (5 LARGE BOXES X 0.20 SECOND = 1 SECOND)
 Voltage 1
- Voltage is important when measuring the height or depth of a waveform.
- The height or depth provides an indication of the amount of electrical activity occurring within the heart.
- Voltage can be affected by a number of different factors to include the amount of viable muscle mass in the heart.
- When analyzing cardiac tracings, the question always comes up “where do I measure from”?
Voltage 2
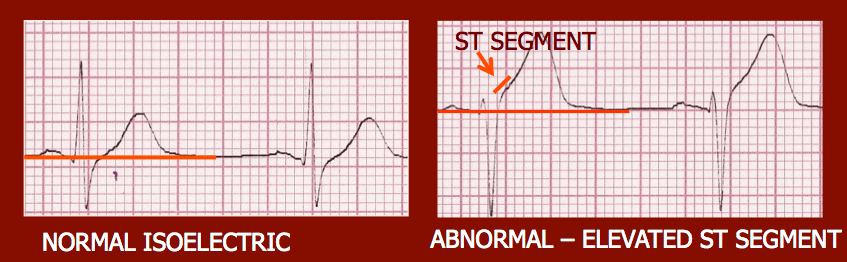
- To keep it as clear as possible, it is important to establish the isoelectric line or baseline.
- There are times when this can prove to be impossible, but in most cases if you can see the PR segment, ST segment and TP segment, you should have a strong sense that this is where the isoelectric line is located.
- However, all three segments are not always on the isoelectric line
- Where two out of the three of them are located when analyzing horizontally, this is typically where the isoelectric line is located.
 |
|
Step 1 - Rhythm Analysis
Introduction
- When analyzing cardiac rhythm strips it is important to recognize what the cardiac complex represents and what is considered normal versus abnormal.
- The technique and interpretation of cardiac rhythms is a combination of science and art.
- The more you practice rhythm analysis the more comfortable you will be with the process involved and the intuitive aspects of interpretation.
Description
- When a normal heart is beating this is the result of electrical impulses that spread through the atria and then the ventricles in an organized, sequential manner. Atria, then ventricles, atria, then ventricles over and over again.
- When analyzing the tracing you will first check R wave to R wave across the strip. If the intervals vary by 1 ½ small boxes or less the rhythm is considered regular.
- If you take your own pulse now and then again in 10 minutes it is unlikely that your heart rate will be exactly the same number. This is because of a number of factors all working together in an effort to maintain our body within a specific range of “normal”, often referred to as homeostasis.
- R wave to R wave analysis refers to the rhythmicity of the ventricles.
- Now measure the P wave to P wave intervals. This refers to the rhythmicity of the atria.
|
|
Step 2 - Heart Rate Regular
Regular Rhythms
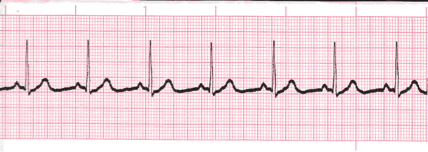
- If the rhythm varies by less than two small boxes, then the rhythm is considered regular.
- The heart rate determination technique used will be the 1500 technique.
- Starting at the beginning of the tracing through the end, measure from one R wave to the next R wave (ventricular assessment), then P wave to P wave (atrial assessment), then count the number of small boxes between each and divide that number into 1500.
-
This technique will give you the most accurate heart rate when analyzing regular heart rhythms. You may include ½ of a small box i.e. 37.5/1500 = 40 bpm (don’t forget to round up or down if a portion of a beat is included in the answer).
 Irregular Rhythms
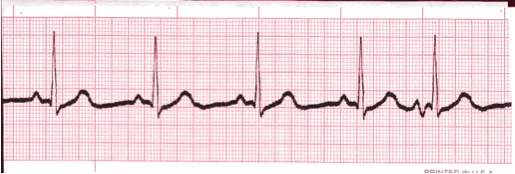
- If the rhythm varies by two small boxes or more, the rhythm is considered “irregular”.
- The heart rate determination technique used for irregular rhythms will be the “six-second technique”.
- Simply count the number of complete cardiac complexes in six seconds and multiply by ten.
 |
|
Step 3 - P wave Morphology (Shape)
Description
- The lead most commonly referenced in cardiac monitoring is lead II.
- For the purposes of this training module, lead two will specifically be referenced unless otherwise specified.
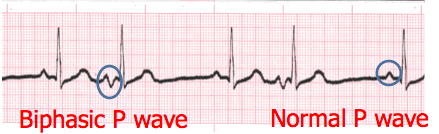
- The P wave in lead II in a normal heart is typically rounded and upright in appearance.
- Changes in shape must be reported. This can be an indicator that the locus of stimulation is changing or the pathway taken is changing.
- P waves may come in a variety of morphologies i.e. rounded and upright, peaked, flattened, notched, biphasic (second complex, pictured), inverted and even buried or absent!
- Remember to describe the shape. This can be very important to the physician when diagnosing the patient.
 |
|
Step 4 – PR interval (PRi)
Description
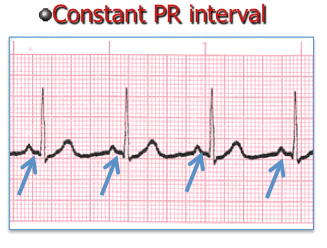
- Measurement of the PR interval reflects the amount of time from the beginning of atrial depolarization to the beginning of ventricular depolarization.
- Plainly stated, this measurement is from the beginning of the P wave to the beginning of the QRS complex.
- The normal range for PR interval is: 0.12 – 0.20 seconds (3 to 5 small boxes)
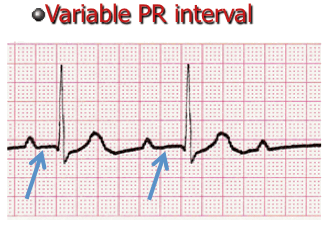
- It is important that you measure each PR interval on the rhythm strip.
- Some tracings do not have the same PRi measurement from one cardiac complex to the next. Sometimes there is a prolonging pattern, sometimes not.
- If the PR intervals are variable, report them as variable, but note if a pattern is present or not.
 |
|
Step 5 – QRS Complex
Description
- The QRS represents ventricular depolarization.
- It is very important to analyze each QRS complex on the tracing and report the duration measurement and describe the shape (including any changes in shape).
- As discussed earlier in step 3, when referring to P waves, remember changes in the shape of the waveform can indicate the locus of stimulation has changed or a different conduction pathway was followed. It is no different when analyzing the QRS complex.
- The difference is that in step 3, we were looking at atrial activity. Now we are looking at ventricular activity.
-
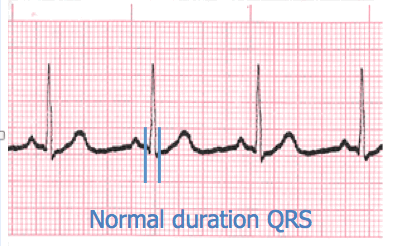
Measure from the beginning to the end of ventricular depolarization.
 Description 2
- The normal duration of the QRS complex measures from: 0.06 – 0.10 second
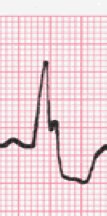
- When the QRS measurement is 0.12 seconds or greater it indicates a delay in the electrical impulse as it is passing through the ventricular conduction system
- Abnormal duration QRS
 |
|
Closing
Interpretation
- The previous slides presented the five-steps of cardiac rhythm strip analysis. These five steps must be followed regardless of how simple of complex the tracing is you are reviewing.
- The information gathered in these steps are telling a story.
- The title of that story is the interpretation.
Irregular Rhythms
- In our other modules on this website, you can learn about the features of different dysrhythmia categories and specific criteria for each dysrhythmia within a category.
- Regardless of the category or dysrhythmia, it is important to always follow the discipline of the five-step rhythm analysis technique.
|